The scariest part of Moose’s recent dental abscess surgery was the anesthesia. After Falcon died, I began hearing a number of veterinary mistake horror stories, many of which were related to deaths caused by anesthesia. While the specifics of each case varied, the narratives generally fell into one of two categories.
- Inappropriate dose/medication – the dog/cat dies on the operating table, sometimes prior to the surgery. In the cases where the pet owner did an autopsy, the report showed the vet used an inappropriate amount or type of medication than was required for that pet.
- Death After the Surgery – the pet owner receives a call from the veterinary clinic after the surgery to report that the surgery went well, that the dog/cat is recovering and should be ready for pick up later that day. When the pet owner goes to the vet to pick up their beloved pet, the vet informs them that the pet has died.
The explanations vary slightly, but in most cases, somebody at the vet mutters something about an allergic reaction to the anesthesia – a rare and completely unpredictable complication. Their pet just happened to be one of the unlucky ones who had a reaction and unfortunately passed away. In some cases, the pets are older, and the death is attributed to their age and/or a pre-existing health condition. But a surprisingly large proportion of the reported deaths are in young, healthy pets going in for spay/neuter procedures or teeth cleanings.
I want to emphasize that the stories I’ve heard are personal stories, often shared with me after somebody learned about the death of Falcon due to veterinary misdiagnosis and neglect. I know many, many pet owners who have pets that have been spayed/neutered without issues or who have undergone surgical procedures with heart conditions and advanced age with no problems whatsoever. But, the proportion of anesthesia-related death stories I heard after Falcon’s death was striking. Why was death from anesthesia so high amidst this select, unscientific gathering of people who have tragically lost their pets? In my line of work, I’ve done a good amount of research related to medical errors in humans. And while the number of preventable deaths or injuries related to mistakes in human medicine is frighteningly high, I can’t remember a single anecdote about death by anesthesia. I know it happens in human medicine, but the volume of veterinary anesthesia horror stories I heard was alarming. And the stories of unnecessary loss were devastating and frightening.
How do I keep my dog safe during anesthesia?
When we chose to bring home such a tiny dog, we knew that Moose’s size would bring with it risks, one of which was anesthesia. As he approached his first birthday, we spoke with our vet about the risks/benefits of neutering such a small puppy (2.5 pounds). Our vets (a husband and wife team who own and run a small clinic in Arlington, VA) talked us through the risks/benefits of the surgery. The biggest risk, of course, is anesthesia. Because of his size, they felt they did not have sufficient experience anesthetizing such a small dog and that they weren’t comfortable using anesthesia with Moose. They gave us the names of several larger clinics that would have more experience with dogs of Moose’s size and would be better equipped to perform the procedure safely. But our vet strongly recommended we consider taking Moose to a hospital associated with a veterinary school, so that the anesthesia would be overseen and administered by a board-certified veterinary anesthesiologist. Then she told me something I found shocking – very few vet clinics actually have an anesthesiologist on staff and in most cases, the anesthesia is administered by a veterinary technician. While there are many excellent, well trained veterinary technicians, not all states require them to be licensed. Most had been trained on anesthesia, and many were very experienced in dosing dogs and cats for a variety of surgeries. But, regardless of experience, the level of training and licensing seemed frighteningly low, especially compared to human medical standards. No wonder I had heard so many deaths by anesthesia stories!
Moose was healthy and the risk of our 2.5-pound, city-apartment-dwelling Maltese finding a female dog small enough for him to hump, while she was in heat, is pretty minimal. So, my husband and I did what every frightened, busy, hyper-analytic dog owner would do. Think about it. (I’ll discuss why I’m not sure this is smart on a later blog post.)
When we learned that Moose had a tooth abscess that would no doubt require surgery, we knew we had to confront the anesthesia issue. While I knew that there would always be risks associated with anesthesia, I was determined to learn as much about the process as possible, so that I could be sure that his care was the best we could find. I put on my patient advocate hat, and I got to work.
I started with friends, asking anybody and everybody I knew who had a pet or was involved with pet care if they had experiences with anesthesiology and any tips that I should take into consideration. I emailed a Yahoo news group of other Maltese owners that Moose’s breeder moderates, asking for advice, suggestions and any information resources that might be helpful. I received some helpful suggestions, but I needed more.
From there I went to google, scouring pet-related Web sites and blogs, looking for tips, suggestions and advice. When that turned up surprisingly little information, I went to the veterinary professional societies. There I got lucky: Both the American College of Veterinary Anesthesiologists and the American Animal Hospital Association had both recently released guidelines for anesthesia and anesthesia monitoring. I reviewed the information in detail and found some articles that were written when the guidelines were released. I found some incredibly helpful overviews of procedures and standards of care, as well as a number of interesting facts and figures (More on that in my related post.) One thing that was missing from these documents, however, was basic background on what the process of delivering the anesthesia entailed. What were the steps, and what types of medications would be used? I tried finding journal articles, but I could find no general review articles on the process, only articles about research into specific anesthesia issues.
Through a friend, I made contact with an incredibly helpful, understanding dog owner who also happened to be a member of the faculty at Cornell Veterinary School. She was very helpful in walking me through the process of delivering the anesthesia. Since I couldn’t find it anywhere else, I’ve provided my notes from the overview she provided during our conversation. (Please note: I’m pretty sure this is an accurate representation of what was described, but any mistakes are no doubt related to my note taking and/or inability to read my own handwriting, rather than that of the gracious interviewee.)
Administering Anesthesia: Process and Protocol Overview
- The process begins with a sedative to calm the dog, typically ketamine with Valium or dexcetomidine (which helps with pain).
- Once sedated, the anesthesiologist inserts an IV into the dog’s vein, typically on the front leg.
- Once the IV is inserted, the anesthesiologist will give an IV injection of something to knock the dog out, so they can intubate him – very brief acting, such as propofol.
- Once intubated, the anesthesiologist administers a gas-like anesthetic. The gas tends to be a very safe drug, such as isofluroine or civofluorine.
- During the procedure, the surgeon/anesthesiologist will often administer some type of pain medication, which helps decrease the amount of anesthesia needed to keep the patient under.
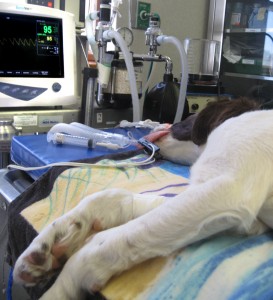
- Throughout the process and the procedure, the surgery team will monitor the patient very closely, looking for changes in blood pressure and peripheral oxygen levels. If the blood pressure or oxygen levels begin to drop, they can administer IV fluids to help stabilize blood pressure before it becomes an issue.
- In addition to a visual monitor, the surgical team would likely have an audible monitor of heart beat, which helps the team detect any changes immediately, based on the audible rhythm of the patient’s heart.
She also suggested that the team would likely insert a stethoscope and EKG monitor through the intubation tube, so that they could get the most accurate measure. When I asked the anesthesiologist at the University of Pennsylvania about this, I was told they no longer did this, because the equipment would occasionally send off sparks or shock the patient. Instead, they used electrodes attached to sticky pads similar to what they use for human EKGs, with the pads being stuck to the dog’s paws.
Armed with this insight and information, I felt much better about my ability to advocate for Moose and ensure that the quality of care he would receive was consistent with clinical guidelines and best practices. Prior to leaving for the hospital, I printed copies of both sets of guidelines, my notes from the conversation with the vet from Cornell, a couple of select articles on veterinary anesthesiology and my list of questions and prepared folders for me and my husband to have for quick references. I also downloaded them onto my iPad, which I made sure was fully charged, in case I needed to google specific issues or questions while at the hospital.
Meeting the surgical team
When we met with the doctors the day before the surgery, I made sure that I met not only with the dental surgeon, but also with the anesthesiologist who would be overseeing Moose’s care. In fact, I met with the head of anesthesiology for the University of Pennsylvania Veterinary School and hospital, Dr. Paula Larenza, who was incredibly helpful. She spent an hour with me, giving me a tour of the facilities, talking through and answering my many questions, showing me their monitoring equipment, safety checklists, emergency preparedness protocols and introducing me to some of the surgical nurses and support staff. In addition, she gave me her email and told me to feel free to email her with questions or concerns.
By the time we left the hospital that day following Moose’s evaluation, I felt very hopeful and reassured. They had demonstrated a willingness to answer all of my questions about quality of care and in fact had encouraged me to ask more if needed. They were not dismissive, patronizing or arrogant. They seemed encouraged by my commitment to ensuring Moose’s care was the best possible, and I felt like they were with me in my efforts to keep my special little puppy safe and healthy. I was still nervous about the surgery. There are no guarantees. But, I felt like the ground was laid for Moose’s surgical team to do the best job they could do for Moose the following morning when we brought him in for the procedure.
I was truly impressed with the care Moose received at the University of Pennsylvania Mathew J. Ryan Veterinary Hospital. The doctors and support team were wonderful. While I don’t have the names of everybody that supported Moose that day, I’ve listed the names that I do have below. I am thankful to each of them for the quality of care they provided to Moose:
Dr. Robert Menzies, Dental Surgeon
Dr. Paula Larenza, head of anesthesiology for UPenn Veterinary school and hospital
Dr. Manuel Boller, anesthesiologist attending
Dr. Joaquin Araos, anesthesiology resident
Teresa Scott, anesthesiology and surgery technician
Jennifer Wintergrass, fourth year veterinary student




I just lost my 7mo old puppy from pre anesthesia sedation being preped for a routine neuter. My heart is broken.
I’m so incredibly sorry to learn of your loss. It’s devastating, and unfortunately, it’s not uncommon. There is so little oversight over veterinary practices. While most vets are conscientious professionals, few have board-certified anesthesiologists who administer their anesthesia. Typically, the anesthesia is dosed and delivered by veterinary technicians who in some states are not licensed. Even the best professionals make mistakes. That’s why I posted this series of stories, hoping to help pet parents prepare for and advocate for their pets during veterinary procedures. I’m so sorry that you lost your puppy. Thank you for your comment.
Got the worst call today. After waiting years to finally get a dog for our family, making sure the kids were old enough, making sure I could be home for the pup, feeling that a dog was like a baby and wanting to provide the best home possible….we got Buoy, a 10 week old chocolate havanese over April vacation. He was a bundle of energy and brought us much joy. We had him for 5 weeks. Yesterday he got his tongue stuck in the tiniest of slots in our kitchen and the removal caused his tongue to tear. After rushing him to the vet and him being observed for hours, he was sent home with plans to stitch the tongue today so that he had fasted and neuter him (as his testicles were already there) at the same time rather than put him through that a few weeks later. He was in great spirits today. When the vet called with bad news, I thought that maybe the tongue didn’t look right or something to that effect. I never ever expected our 15 week old puppy to die. Dr. said surgery went fine but that Buoy’s heart arrested when coming out of anesthesia. Got him back once but then it happened again and they could not resuscitate him. We are devastated. I have asked for the medical records, but should I request an autopsy as well. Would there be anything to bring us comfort in that or would it just be prolonging our grieving. We don’t know what to do.
Jane – I am so incredibly sorry to learn about your loss. I truly understand how devastating that can be. I would get as much information as I could from your vet, and I would inquire about their monitoring practices post-anesthesia, which is often when problems occur. Vet practices are often understaffed for the post-procedure monitoring, and it doesn’t take long for things to go drastically wrong.
As for whether or not that will prolong your grieving? I can’t say. I know that nothing you do will bring your puppy back. I still think of Falcon every day. However, while the steps I took after Falcon died didn’t bring him back, I did, at least, get the vet to pay the costs of the procedures and “replacement costs” for Falcon – a term which sickens me, but is at least something. The Vet also changed their procedures and did an internal seminar about what they did to cause Falcon’s death. For me that was a little bit of closure, but it did take a lot of effort to make that happen. Only you can weigh the costs/benefits for you and your family. I wish there were a more straightforward response.
Again, I am so very sorry to learn about your puppy’s death. For what it’s worth, my husband kind of ‘forced’ me to get Moose after Falcon died. I thought it was a bit too soon, but it was truly the right decision for us. He is his own little character and reminds us of Falcon in many ways. It was a very healing experience for my husband and me, and I can’t imagine life without Moose.
Let me know what you decide. I wish you well! – Anna
We lost our 9 year old yorkie when he died after routine teeth cleaning. Apparently they had finished the procedure (1.5 hours which I feel was too long for a 3.5 kg yorkie) when his heart stopped. Resuscitated but his heart stopped again. We are absolutely devastated as he was our baby and in perfect health.
I’m so sorry for your loss. It’s so devastating. My thoughts are with you! – Anna
My one year yellow lab was sick and she had to have and exploratory surgery and everything came out fine until the next day I got a called from the vet that she didn’t make it through the night or morning cuz they left her unattended all night so they don’t what time she passed away in my heart and opinion I think they put her down or died of an allergic reaction to the anesthesia and I wasn’t told she didn’t look like she got and iv because two days prior she had blood work done and the same bandage was on the same paw
Maria – I’m so sorry to learn about the loss of your yellow lab. It’s a far too common story. After anesthesia, it’s critical to monitor the vital signs of pets (or people!) very closely, and often local vets don’t have the staff support needed to provide the attention and monitoring needed. That’s why I take Moose and Buckley to a veterinary school/center of excellence, but that’s not possible for many of us. Again, I’m sorry for your loss. Be well. – Anna
I just lost my Stella, 14 month old pit that had her liter ,they were 8 weeks. I took her in to a vet I have used before, for Stella’s spay . I got a call , she did fine pick her up around 4 that day (yesterday 6th) I got her home at 5:30 we moved her bed in spare room so she could be away from the 2 puppies, she seized , I called the on call got her there , she kept seizing about 7 times , they said she was probably braindead and we needed to make a decision, well knowing her she would want peace. She passed at 9:20 last night. Now how can a healthy , all her shots, gave birth to 11 babies one passed. I gave her multivitamins the day she conceived until yesterday. Stella stayed inside , her babies also. I don’t understand, I need help finding answers. Thank you
Michelle – I’m so sorry to learn of your loss of Stella. It really is so devastating. I don’t know if it was linked to the anesthesia, but I hear of so many similar cases of what seem to be preventable deaths. I hoped in writing these blog posts that I could help pet owners/parents advocate in advance of their surgeries, but too often they read the articles after something tragic has happened. We don’t look for answers unless we think we need them, and as I learned with Falcon, sometimes that’s too late. I wish I could say something to ease the loss, but know that you are not alone in your grief. Be strong and well. – Anna
I share everyone’s heartbreak. After 15 wonderful years we finally lost our beloved male Miniature Schnauzer. Several months later my husband bought me a gorgeous puppy as a Christmas present. He was the most affectionate and happy dog we ever had and we both were in love with him. At nine months we took him to our regular vet for neutering. Everything went well until he started coming out of the anesthesia, when his heart stopped. Nothing that they tried could bring him back and we lost him. We don’t know why it happened and our vet is at a loss to explain it.
We both cried for days.
How incredibly heartbreaking. I’m so sorry for your loss.
Today I to received the most heart wrenching phone call. My five month old German shepherd was to be spayed. She went in cardiac arrest and passed. The vet said she was doing fine but when they turned her on her back and started to make an incision she went in arrest. She was so full of energy and healthy. I am devastated
I’m so sorry. It must be devastating. My thoughts are with you. – Anna
Molly, my 6 month old lab, when in today to be spayed. About 4 hours later, I got a call that she died on the table…they resuscitated her and she is now flat out in a kennel. Don’t know what will happen next. Originally, when I asked the vet, I was told she was without oxygen to her brain for about 1 1/2 to 2 minutes. This afternoon when I went out to see my Molly….the vet admitted she had no idea how long it took to get her breathing again. I was told most likely an allergic reaction to the anesthesia. The vet also wondered aloud to me, that perhaps there was a heart issue. I requested all pre-op blood work…which I was told showed normal. Don’t know about tomorrow morning….
My sincere apologies for my slow reply! I’m so sorry to learn about this. I hope Molly recovered, and I would love an update. We all need to learn from one another’s experiences, as well as share one another’s grief. Thanks for your note! – Anna
Hi Anna…I’m sad to say I had to put her to sleep 4 days later…extensive brain damage. I’ve learned much since. My state (NM) does not require a license for techs to administer anesthesia. I believe there was an inexperienced tech and Molly got into trouble before the tech even realized it…Molly crashed almost immediately after the procedure started…the incision was never made. To make matters worse, the vet tried to stick me with a $200 bill for a bunch of piddly little stuff…IV lines, fluids, etc. I declined to pay and told her the honorable thing to do was to help with the purchase a new dog…she declined but did write off the bill.
I’ve since acquired a little chocolate lab, and yes, she was spayed at 6 months at a new veterinary clinic. I asked for a second vet to administer the gas. Other than a very long day for me (!!) we did fine. My advice to everyone…ask questions prior to the procedure. Make sure you are comfortable with the level of expertise of the vet and technicians. In my case, a second vet to administer the gas helped my peace of mind…a lot more expensive, but worth the cost!
Thank you for following up on my post. I was a total wreck that day…and then when I had to decide to say goodby 4 days later…well, my heart was broken. I’ll never know what really happened, but knew I couldn’t live without a furry friend.
I just lost my Boston Terrier yesterday. She went in for bilateral knee surgery. I called to check on her they said everything went well and wanted me to pick her up at 6 pm. Then 20 minutes later I got a call that her heart stop and they brought her back three times and that I need to hurry and get there. The vet said she did good through the whole procedure he doesn’t know what happened that maybe it could be she had a underlying heart disease. I’m in a million piece right now
Hi Pauline – My apologies for my slow reply. I’m so very sorry to learn about this. I know it’s devastating, and it happens all too often, which is why I wrote this series on the blog. I hope you are healing from your loss. Best wishes – Anna
Thank you for the information. My little Ti Amo is only 2.5 lbs and I am very concerned of the anesthesia during his surgery to get him neutered. I feel more confident and geared with better questions to ask the vet when I go in to make his appointment. Thank you for sharing.
I took my 3 year old male GSD to the vet to be neutered today. They administered acepromazine and atropine. He died on the floor before they even began the operation. He was perfectly healthy when I took him in with no past illness. Blood work came back normal. Chest X-ray didn’t show anything. The vet had no explanation. We sent him for toxicology and autopsy. I will get justice for my baby boy!
Thank you for sharing your experience and knowledge. When we adopted our adorable little puppy from AC 4 years ago, we decided not to put her through the trauma of surgery and to deal responsibly with her heat cycles. They only happen about every 6 months and have been easily manageable, with no opportunity for a pregnancy. But we’ve been discussing whether spaying might be better for her in the long run. However, the risk of death from anesthesia–the thought that we could lose this precious little girl on the operating table is just unbearable. My research has just begun.
I took my 3 year old cat in to be groomed and they gassed him to death and then revived him but said he might be brain damaged. I brought in a happy and healthy cat and brought home a pet that can’t hear, see or walk. The vet said he would not stop struggling so they gassed him good. Not only did they not give us a discount on the vet bill but they charged us more than what they quoted us. The sad part is they charged us extra for reviving Archie after they killed him. We went to a lawyer but they told us that the vets are not responsible if your pet dies or gets injured. That needs to change. Now we go to a neurologist to see if he can reverse the damage that thevet did to him. Truly heartbreaking!!
I just lost my 2yr old Hani, healthy rambunctious baby boy that he was, he went in for a teeth cleaning, when I picked him up his skin was ice cold and he was shivering. He developed a cold the next day sneezing and coughing with discharge. I called the vet twice with my concerns and they said he was under a lot of stress during the procedure , but the cold was nothing to be worried about, I came home to find him dead.The vet performed an necropsy and told me his best guess was that he had heart disease. My heart is so broke, that I placed my baby in harms way, that he suffered at the hands of a careless animal hospital.
We just lost our 7 yr old morkie Aaron after he had his routine teeth cleaning. He was perfectly healthy. The vet told us that he probably had an underlying condition. They said he came out of the anesthesia fine then looked up. Once they removed the tube he passed away. Not knowing what really happened to him is devastating to my whole family including my 10 yr old yorkie. They were best friends.
Just reading all this sadness has me crying. My sweet little baby shih tzu is 7 months old and only 4.5 lbs. She has to have surgery on some teeth issues and will be spayed at the same time, just one week from now. IM SO SCARED!!! She’s so tiny, so fragile, so sweet!! ❤️🐶❤️😬
I am sorry I’m just seeing this post. I hope your Shih Tzu’s surgery went well and that perhaps this blog series was a helpful tool for you and her. Please reply with an update. – Anna
We just had our beautiful almost 2 year old German Shepherd neutered and he died at home at 4:30am. Why????? We noticed that he was really out of it in the evening, but didn’t think much of it. Then I heard his body drop outside my bedroom door at 4:00am. 30 minutes later he stopped breathing. Just unreal.
I am so sorry to learn about the loss of your German Shepherd. I know how devastating that can be. Thank you for sharing your story. – Anna
We took in our healthy 7 month yorkie to get spayed yesterday and got a call from the vet that she died after surgery. It sounds as though they gave her too much medicine. Is there anything we can do?
I am so very sorry to learn about the death of your puppy. I know how devastating it can be. At this point, I’m not sure what you can do. You can quiz the vet about their post-surgical monitoring procedures and staffing, but there is very little that pet parents can do to hold vets accountable – or for that matter to truly understand what, exactly, went wrong. I wish I could give better guidance. Again, I am sorry to learn about your loss. – Anna
Just lost my 8 month old, Luca, after surgery. A mini- Doberman that brought us so much joy. I got the phone call that everything went well and he was in recovery. A bit later, I got another call- he’d gone in to cardiac arrest. They performed CPR but couldn’t get him back. I’m devastated and full of guilt. This is a new vet to us- as our long time vet just retired. The new vet has years of experience and a great reputation. But, routine labs weren’t done. I thought they were automatic, but aren’t. I know they don’t show everything, but as an RN- I feel terrible. If nothing else- if I’d advocated for Luca, maybe I’d not have the burden of all this guilt.
I am so very sorry to learn about Luca’s death. Unfortunately, it’s not an uncommon story. The procedure goes well. The pet parent receives a call that their dog or cat is “recovering”. Then they receive a second call saying something went wrong and the animal has died. I don’t know the specifics of Luca’s case, but the research I’ve done suggests that the issue is often related to poor or inadequate monitoring of the dog while he/she is in recovery from the anesthesia. It is critical that any animal – or person – be very closely monitored throughout their recovery from anesthesia. While many vets do this well, some do not staff appropriately for this critical part of the process. And, in some cases, that failure to staff can be deadly. I’m so very sorry for your loss. Best wishes – Anna
My 12&1/2 year old cat had to have surgery to remove his gallbladder yesterday…his heart stopped on the table but they got him back…she said he was out for around 1 min but he is not coming out of the anesthesia right & showed no visable sign of recognizing me…he would move his head a little & blink when I petted him on the side of his face…this is 18 hrs after surgery…do you think he might have brain damage?
I am not able to assess if your cat has brain damage, but I sincerely hope he has recovered and is doing OK. Thanks!
I lost my beautiful cat Pippa last Thursday 19th July 2018, she died whilst in recovery from anesthesia for dental cleaning/extraction. They said in recovery she was struggling to breathe, then her heart stopped, they tried to resuscitate her but couldn’t. I am in shock, completely devastated and heartbroken. From doing research since (this is how I found this site) I am shocked there appears to be so many deaths from anesthesia, I didn’t realise the risk is 1 in 1000 for cats, I thought it would be 1 in 100,000 or something. I don’t understand what went wrong and why my cat died, she had had anesthetic before on 2 previous occasions with no problems. She was older this time at 13 and her appetite had been decreased for a few weeks, both I and vet thought it may be due to sore teeth, so I agreed on the procedure. If only I could go back and change my decision, but I’ve had toothache and abscesses and it was the worst pain ever, so I didn’t want that for my girl. I’m trying not to blame the vets but it’s hard because a natural part of grieving is blame, you blame yourself as well as others involved. The loss of our fur baby’s is so painful and upsetting and surely in 2018 it should be much more preventable than it seems it currently is with such advances being made in medicine.
Good luck getting people to pay prices for a place who pays anesthesiology residents. In Idaho our fb pages constantly complain about prices and want to find cheapest dr in town. Laws don’t require them but that doesn’t mean the vets don’t know what they are doing. Out of thousands a year maybe one death. It is horrible I agree but people need to do like you and think is this procedure necessary and worth the risk. Death can occur even with an anesthesiologist on staff.
I lost my 13 month Chihuahua Ted yesterday during routine neuter. He crashed whilst under anaesthetic. They resuscitated him but he had been gone 10 minutes. The brain damage was too much as he was fitting constantly. I got to say good bye and he was out to sleep in my arms. I’m devastated.
I am so very sorry for your loss. It’s never easy, but it’s so much more difficult when they are young, healthy and their death is preventable.